“Your mind is in every cell of your body.”
—Candace PertIn part 1 of this series we reviewed the classic definition of the manipura chakra, examined the forms and functions of the tissues associated with it, and introduced the gut microbiota and the gut-brain axis. In part 2 we will explore the amazing collection of cells known as the gut microbiota—their innate consciousness and how they influence the mind and body.
The Microbiota
The massive collection of bacteria cells located throughout the body is known collectively as the microbiota. These bacteria number approximately 38 trillion, with the majority located in the digestive system. The gut microbiota is the collective name given to this colony of bacteria lining the intestinal tract. Rather than being parasitic or simply coming along for the ride, these cells assist with digestion and assimilation, especially of food compounds that are otherwise difficult to digest and absorb. These bacteria also synthesize amino acids, as well as B vitamins and vitamin K. In addition, gut bacteria play a crucial role in immune system regulation. Most important, the gut microbiota interacts with and influences the central nervous system (CNS, or the brain and spinal cord). In order to understand just how miraculous and powerful this collection of cells is, let’s begin with the individual unit that comprises the whole: a bacterium, or single cell of bacteria.
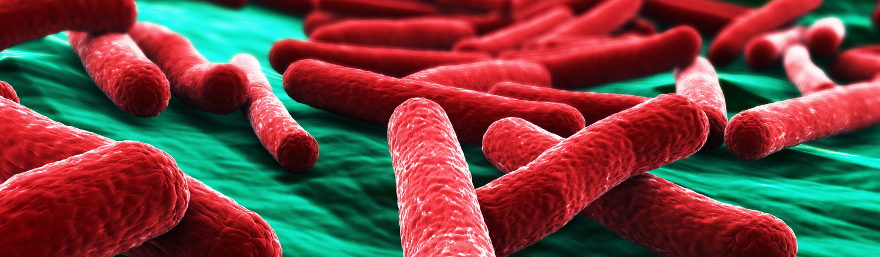
Bacteria are among the smallest units of recognized life, a group known as single-celled organisms. In fact, bacteria are so “stripped down” that they don’t contain any internal structures (such as a nucleus and mitochondria), unlike white blood cells and nerve cells, for example. Despite this, these cells are extremely sensitive and adapt to changes in their environment, indicating the presence of some sort of primitive sensory system. Bacteria communicate with each other and their environment by using a variety of chemical signaling molecules. These individual sensory and signaling systems become immensely powerful when they are integrated into the greater collective of the gut microbiota.
When in a colony, bacteria act like a true multicellular organism. They alter their behavior in a coordinated way based on changes in the environment, and on what the community as a whole senses, via a mechanism called quorum sensing. This is a stimulus and response system, correlated with the population density of the bacteria, which regulates their genetic expression and thus their characteristics and behavior. This collective consciousness doesn’t just affect the local environment of the gut, it also influences the impulses sent to the central nervous system. In turn, impulses from the central nervous system affect this networked consciousness. This powerful two-way communication system is known as the gut-brain axis.
The gut-brain axis is the signaling pathway between the gastrointestinal tract and the central nervous system. It includes the brain and spinal cord, as well as the solar (celiac) plexus and the vagus nerve (both of which we discussed in part 1, including their associations with the sympathetic and parasympathetic divisions of the autonomic nervous system). The gut-brain axis also includes the hypothalamus and the pituitary and adrenal glands (the HPA axis)—the foundation of the system responsible for our fight or flight response.
The bacteria of the microbiota synthesize a broad range of chemicals that interact with and change the environment of the gut and communicate with the emotional and cognitive centers in the brain via the gut-brain axis. Many of these chemicals are neurotransmitters and hormones. The vast toolbox of psychobiological chemicals the microbiota synthesizes includes:
Acetylcholine
Acetylcholine is the primary neurotransmitter that activates the parasympathetic (rest, digest, heal, and reproduce) division of the autonomic nervous system. It stimulates the relaxation response by decreasing heart and respiratory rates and increasing digestion and elimination. It also plays a crucial role in cognition, memory, and learning, and is the principal neurotransmitter involved in muscle contraction and movement.
Dopamine
Dopamine plays many roles. Outside of the brain, its functions are mainly hormonal in nature—reducing peristalsis in the digestive tract and protecting the intestinal lining, as well as helping to regulate the kidneys, pancreas, and immune system, and acting as a vasodilator. In the brain, where dopamine is produced separately from the dopamine produced in the gut, it is a neurotransmitter associated with the brain’s reward and pleasure centers and with regulating movement and emotional responses.
Norepinephrine
Norepinephrine, or noradrenaline, acts as a neurotransmitter and a hormone in activating the mind and body. It stimulates the fight or flight response of the sympathetic division of the autonomic nervous system, promoting focused alertness as well as elevating heart rate, blood pressure, and respiratory rates, and increasing energy production. At the same time, it inhibits digestion by decreasing gut motility, or peristalsis, as well as blood flow and secretion of digestive juices. On the level of our mind, norepinephrine increases the potency of our memories, ensuring accurate memory recall.
Gamma-Aminobutyric Acid (GABA)
GABA is a powerful neurotransmitter that calms the mind and relaxes the body. It also increases peristalsis and secretion of digestive juices. Practicing yoga has been shown to increase the production of GABA, decrease anxiety, and improve mood.
Histamine
Histamine is a chemical with several hormonal and neurotransmitting functions. It is involved in, among other things, immune response and inflammation, smooth muscle contraction, and regulating certain aspects of the gut such as gut permeability and the secretion of digestive juices.
Serotonin
Serotonin is one of the primary hormones the body uses to communicate the state of gut health to the CNS. Ninety percent of the body’s serotonin is located in the gut, where it stimulates and regulates peristalsis. Too much serotonin in the lining of the gut causes hypermotility, or diarrhea; too little contributes to constipation. The remaining 10 percent of the body’s serotonin regulates mood, appetite, and the sleep cycles. Balanced serotonin levels elicit feelings of relaxation and wellbeing and assist in digestion, elimination, learning, and memory.
Melatonin
A healthy gut microbiota will release hormones that affect us in a positive way.
Melatonin is a hormone that impacts a number of functions within the body, but it is best known for its regulation of our circadian rhythm and sleep cycles. The importance of melatonin to gut function and health is evidenced by the simple fact that, at any one time, the gut contains at least 400 times more melatonin than the brain. In the gut, melatonin stimulates peristalsis and immune system function and protects against inflammation.
Gut Health and the Manipura Chakra
To summarize what we have examined so far, a well-functioning, healthy gut microbiota will release a level and combination of hormones and neurotransmitters that affect us in a positive way, supporting our health and sense of wellbeing. Of course, if the gut microbiota is in a weakened or imperiled state, the opposite will be true. The manipura chakra helps us digest and assimilate what we take in from the world, both physically and mentally. If the microbiota is unhealthy, these digestive, transformative functions of the manipura chakra will similarly become impaired and sluggish, negatively affecting our vitality. A healthy microbiota helps us live a more vibrant, radiant life.
Further Reading
Armitage, J. P. (1992, February). Bacterial Motility and Chemotaxis. Science Progress, 76 (301–302 Pt 3–4), 451–477. Abstract available at https://www.ncbi.nlm.nih.gov/pubmed/1364581.
Carabotti, M., et al. (2015). The Gut-Brain Axis: Interactions Between Enteric Microbiota, Central and Enteric Nervous Systems. Annals of Gastroenterology, 28(2), 160–172. Retrieved from http://www.annalsgastro.gr/index.php/annalsgastro/article/view/1959/1537
Chen, C. Q., et al. (2011, September 14). Distribution, Function and Physiological Role of Melatonin in the Lower Gut. World Journal of Gastroenterology, 17(34), 3888–3898. Retrieved from https://www.wjgnet.com/1007-9327/full/v17/i34/3888.htm
Clark, G., et al. (2104, August). Gut Microbiota: The Neglected Endocrine Organ. Molecular Endocrinology, 28(8), 1221–1238. Retrieved from https://academic.oup.com/mend/article/28/8/1221/2623221
Eisenhofer, G., et al. (1997, November 1). Substantial Production of Dopamine in the Human Gastrointestinal Tract. The Journal of Clinical Endocrinology & Metabolism, 82(11), 3864–3871. Retrieved from https://doi.org/10.1210/jcem.82.11.4339
Encyclopædia Britannica website editors. (2017). Histamine. Retrieved from https://www.britannica.com/science/histamine
Ercan, F., et al. (2004, September). Role of Melatonin in Reducing Water Avoidance Stress-Induced Degeneration of the Gastrointestinal Mucosa. Journal of Pineal Research, 37(2), 113–121. Abstract available at http://onlinelibrary.wiley.com/doi/10.1111/j.1600-079X.2004.00143.x/abstract;jsessionid=E7C063A1EC3B4FE51FF58077D32D4428.f04t03
Petra, A. I., et al. (2015, May 1). Gut-Microbiota-Brain Axis and Effect on Neuropsychiatric Disorders with Suspected Immune Dysregulation. Clinical Therapeutics, 37(5), 984–995. Retrieved from http://www.clinicaltherapeutics.com/action/doSearch?searchType=quick&searchText=Gut-Microbiota-Brain+Axis+and+Effect+on+Neuropsychiatric&occurrences=articleTitle&journalCode=clithe&searchScope=fullSite
Sender, R., et al. (2016, August 19). Revised Estimates for the Number of Human and Bacteria Cells in the Body. PLOS Biology, 14(8). Retrieved from http://journals.plos.org/plosbiology/article?id=10.1371/journal.pbio.1002533
Streeter, C. C., et al. (2010, November). Effects of Yoga Versus Walking on Mood, Anxiety, and Brain GABA Levels: A Randomized Controlled MRS Study. Journal of Alternative and Complementary Medicine, 16(11), 1145–1152. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3111147/
Trewavas, A. J., & Baluška, F. (2011, November 18). The Ubiquity of Consciousness: The Ubiquity of Consciousness, Cognition and Intelligence in Life. EMBO Reports, 12(12), 1221–1225. Retrieved from http://embor.embopress.org/content/12/12/1221
